By Dr Meredith Blampied
It has been very encouraging to observe a growing conversation in the general public about the importance of mental health. This has particularly centred on anxiety and depression, two of the most common and most costly mental health issues.1 2 Celebrities, sports people, business leaders are all speaking up about their own experiences of mental illness and the importance of reaching out for help. Given the burden on society of these mental health issues, both in terms of treatment and lost productivity, it is crucial that these conversations continue.
However, there are several challenges. Firstly, access to treatment is only getting worse.3 Health treatment rationing is reaching a pinch point in Aotearoa and even if people recognise the need to seek treatment for mental illness, it is not guaranteed that they will be able to receive evidence-based treatments in a timely fashion, particularly if private finances are limited.4 Additionally, even if treatment options are made available, options for effective and safe treatments for anxiety and depression can be limited to medication and/or psychological therapy.5 6 It is time to look beyond psychological therapy and psychiatric medication towards other avenues of treatment, both to increase the availability of safe and effective treatments, and to give people with anxiety and depression meaningful choices in how to treat these conditions.
The concept of using food and nutrition as a potential treatment for illness is not a novel concept,7 and the recent interest in the gut and the importance of healthy gut function on healthy brain function has generated an increase in studies exploring nutrition and psychology. Research from a variety of trials has demonstrated that the Mediterranean diet can be effective at improving symptoms of depression in people who meet criteria for a Major Depressive Disorder and may also improve symptoms of anxiety.8 9 Studies exploring the efficacy of single nutrients at improving symptoms of mental health have found benefit for zinc,10 magnesium and B6, 11 and vitamin B complex.12 However, there are limitations to the single nutrient or favourite few approaches and an alternative may be found in using the full array of micronutrients called broad spectrum micronutrients, which combine all essential vitamins and minerals.13
In 2018, the Nutrients for Mental Health, Anxiety and Depression trial (NoMAD) started recruiting participants with problematic symptoms of anxiety and/or depression. This was the first double-blind, randomised placebo-controlled trial to explore whether or not a combined vitamin and mineral formula (Daily Essential Nutrients) could improve symptoms of anxiety and depression in people with these conditions. One hundred and fifty people from Ōtautahi participated in the trial, which included a two-week baseline phase (where no nutrients were taking but symptom severity was tracked weekly), followed by a 10-week treatment phase, where participants took either the micronutrients or a placebo. Participants took up to 12 pills a day and reported their symptoms weekly. Side effects were also tracked for the duration of the trial.
The main variables of interest were participants’ report of depressive and anxiety symptoms as well as side effects, given that negative side effects is a consistently reported reason that people withdraw from other treatments for anxiety and depression.14
We are very excited to share the results now that they are published.15 The good news was that most of our participants experienced significant improvements in their symptoms of anxiety and depression, regardless of whether they were taking the micronutrients or placebo. This means that people can improve simply by being actively monitored online. However, participants who were taking the micronutrients experienced improvements more quickly than participants who were taking the placebo (see figures).
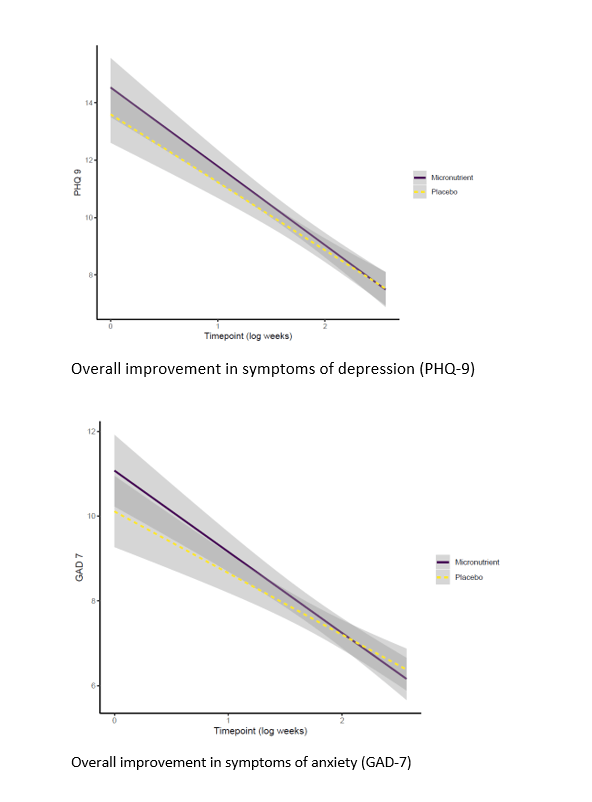
Perhaps more interestingly, there were subgroups who appeared to benefit more from the micronutrients relative to placebo. Specifically, younger participants, people who had previously trialled psychiatric medications, and people from lower socio-economic groups all benefitted more from the micronutrients. This provides useful information to clinicians as to who could be targeted with this intervention.
Encouragingly, with the exception of more gastric upset reported in the micronutrient group (gastric distress is a well-known side effect of taking vitamin and mineral products), there were no significant differences between the placebo and the micronutrient groups in terms of side effects experienced. No side effects were sufficient to cause any participant to withdraw from the trial and no participants experienced any increase in suicidal thinking or behaviour during the trial. This is good news given the recent studies showing the increases in suicidal ideation associated with SSRIs.16 We also had a remarkably low drop out rate at 5%.
Of the people who entered the trial reporting symptoms that likely met criteria for clinical depression, 61% of the micronutrient group and 49% of the placebo group achieved clinically significant improvement. This translates into a number needed to treat (NNT) of 8, comparable to estimates from both SSRIs and TCAs but with fewer side effects.17
Of the people who entered the trial reporting symptoms of anxiety that likely indicated a possible anxiety disorder, 62% of the micronutrient group and 56% of the placebo group showed clinically reliable change. This is equivalent to an NNT of 17.
This study was important in a number of different ways. Firstly, it demonstrated the acceptability of micronutrients as a potential treatment for anxiety and depression and that this is likely a safe intervention for people to take. About half of people benefited significantly from the intervention. Results also showed that the placebo effect does not work as well for some subgroups and that this should be considered when exploring treatment options.
People experiencing anxiety and/or depression have a right to choose a treatment option that feels like a good fit for them, from a range of safe, effective and accessible treatments. The results of the NoMAD trial are both reassuring and exciting and it is essential to promote replication of this research in other research centres.
References
1. Lim GY, Tam WW, Lu Y, et al. Prevalence of depression in the community from 30 countries between 1994 and 2014. Sci Rep 2018;8(1):1-10.
2. Baxter AJ, Vos T, Scott KM, et al. The global burden of anxiety disorders in 2010. Psychol Med 2014;44(11):2363.
3. Rucklidge JJ, Darling KA, Mulder RT. Addressing the treatment gap in New Zealand with more therapists-is it practical and will it work? N Z Med J 2018;131(1487):8-11.
4. Alonso J, Liu Z, Evans‐Lacko S, et al. Treatment gap for anxiety disorders is global: Results of the World Mental Health Surveys in 21 countries. Depress Anxiety 2018;35(3):195-208.
5. Hofmann SG, Asnaani A, Vonk IJJ, et al. The efficacy of cognitive behavioral therapy: A review of meta-analyses. Cognit Ther Res 2012;36(5):427-40.
6. Sanches M, Quevedo J, Soares JC. New agents and perspectives in the pharmacological treatment of major depressive disorder. Prog Neuropsychopharmacol Biol Psychiatry 2021;106:110157.
7. Barroux G. From century to century: Diet at any cost? A glance at a few mentions of diet in the history of medical practices. Journal of the CIPH 2019(2):167-80.
8. Jacka FN, O’Neil A, Opie R, et al. A randomised controlled trial of dietary improvement for adults with major depression (the ‘SMILES’ trial). BMC Med 2017;15(1):23.
9. Parletta N, Zarnowiecki D, Cho J, et al. A Mediterranean-style dietary intervention supplemented with fish oil improves diet quality and mental health in people with depression: A randomized controlled trial (HELFIMED). Nutr Neurosci 2019;22(7):474-87.
10. DiGirolamo AM, Ramirez-Zea M, Wang M, et al. Randomized trial of the effect of zinc supplementation on the mental health of school-age children in Guatemala. The American journal of clinical nutrition 2010;92(5):1241-50.
11. De Souza MC, Walker AF, Robinson PA, et al. A synergistic effect of a daily supplement for 1 month of 200 mg magnesium plus 50 mg vitamin B6 for the relief of anxiety-related premenstrual symptoms: a randomized, double-blind, crossover study. J Womens Health Gend Based Med 2000;9(2):131-39.
12. Young L, Pipingas A, White D, et al. A Systematic Review and Meta-Analysis of B Vitamin Supplementation on Depressive Symptoms, Anxiety, and Stress: Effects on Healthy and ‘At-Risk’ Individuals. Nutrients 2019;11(9):2232.
13. Blampied M, Bell C, Gilbert C, et al. Broad spectrum micronutrient formulas for the treatment of symptoms of depression, stress, and/or anxiety: a systematic review. Expert Rev Neurother 2020;20(4):351-71.
14. Ferguson JM. SSRI antidepressant medications: adverse effects and tolerability. Prim Care Companion J Clin Psychiatry 2001;3(1):22.
15. Blampied M, Tylianakis JM, Bell C, et al. Efficacy and safety of a vitamin-mineral intervention for symptoms of anxiety and depression in adults: A randomised placebo-controlled trial “NoMAD”. J Affect Disord 2023;339:954-64.
16. Lagerberg T, Matthews AA, Zhu N, et al. Effect of selective serotonin reuptake inhibitor treatment following diagnosis of depression on suicidal behaviour risk: a target trial emulation. Neuropsychopharmacology 2023.
17. Arroll B, Elley CR, Fishman T, et al. Antidepressants versus placebo for depression in primary care. Cochrane Database Syst Rev 2009(3):Cd007954.













